Targeting Emergency Department Resources to Address the Opioid Epidemic
How to Have the Greatest Population Impact
This article originally appeared on the University of Pennsylvania Leonard Davis Institute Health Policy$ense blog.
In a new study in the American Journal of Emergency Medicine, my colleagues and I estimate the number and distribution of emergency visits for opioid use disorder (OUD) across the country. We found that nearly 2/3 of all emergency visits for OUD occurred in 25% of EDs nationwide. Why is this important?
Patients with OUD come to the emergency department (ED) for several reasons related to opioid use. The risk of death following an ED visit for opioid overdose is very high (5.5% within a year) and the ED is an accessible setting for MOUD initiation, naloxone distribution, and linkage to care.
However, few EDs provide life-saving buprenorphine or harm-reduction and care coordination services and providers cite many barriers, including the lack of departmental or institutional support.
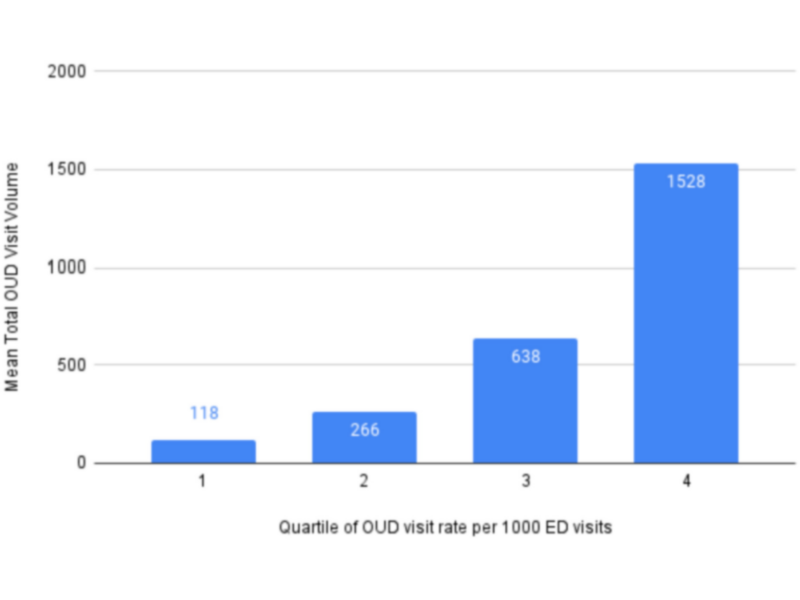
Using data from the Healthcare Cost and Utilization Project, we found that in 2017 there were about 1.5 million ED visits for OUD in the U.S. As shown in Figure 1, there is significant variation in the annual mean number of OUD visits across hospitals. We found that 64% of OUD-related visits occurred in just 25% of the EDs nationwide, mostly in metropolitan areas and teaching hospitals.
Unsurprisingly, there is a moderate correlation between total ED volume and total OUD volume. However, there is not such a correlation between total ED volume and OUD visit rate. If your ED has 23 visits for OUD for every 1,000 ED visits, you are in the top quartile.
Our results suggest that state and local policymakers should identify hospitals with the highest OUD visit rate, which does not necessarily correlate with total ED volume, and target resources accordingly.
As we continue to expand efforts to combat the overdose crisis, targeting our quality improvement efforts to EDs with the highest OUD visit rates could potentially benefit more than half of all patients utilizing emergency care for OUD nationwide.
The study, Variation in emergency department visit rates for opioid use disorder: Implications for quality improvement initiatives, was published in the January 2022 issue of the American Journal of Emergency Medicine. Authors include Utsha G. Khatri, Elizabeth A. Samuels, Ruiying Xiong, Brandon D.L. Marshall, Jeanmarie Perrone, and M. Kit Delgado.