No Safe Dose for That First Opioid Prescription
This post originally appeared on the Health Policy$ense blog at University of Pennsylvania Leonard Davis Institute.
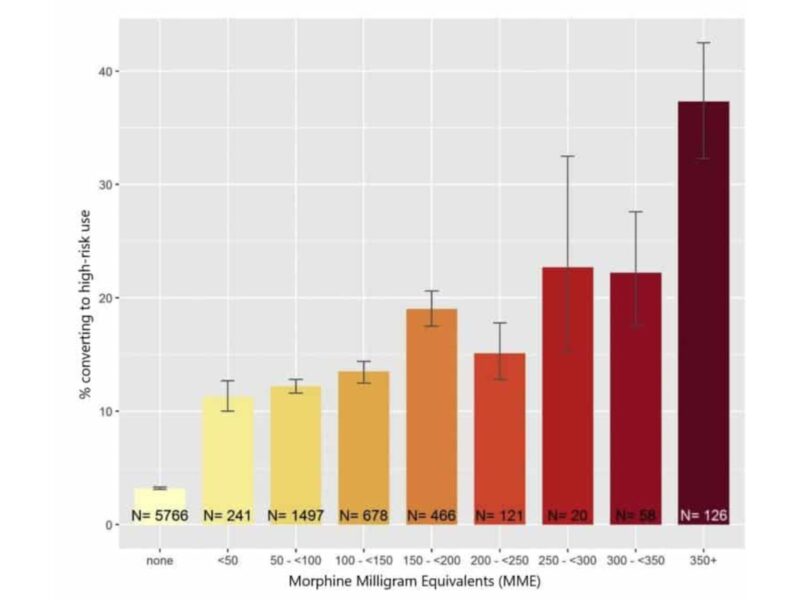
LDI Senior Fellows Zack Meisel, Benjamin Sun, and colleagues have a striking and sobering chart in a recent Annals of Emergency Medicine article on initial opioid prescriptions in the emergency department. They tracked how many “opioid-naïve” patients (i.e., those without a record of opioid use in the previous year) had persistent or high-risk opioid prescription use in the subsequent year.
They studied Medicaid patients seen in Washington State EDs between 2013-2015. Of patients who filled opioid prescriptions within one day of their ED visit, 13.7% converted to persistent or high-risk opioid prescription use, compared to 3.2% who were not prescribed an opioid.
Not surprisingly, the size of the initial ED opioid prescription was strongly associated with continued risky use, as shown in the chart above. While we might tend to focus on the extreme risk faced by those receiving the highest doses, we might also look at the risks faced by the majority receiving up to 100 MME (that’s fewer than 25 tablets of hydrocodone/ acetaminophen 5/300). Although the dosage is well within current CDC acute pain guidelines, these patients still face a risk of more than 10%.
As the authors state, “…there is no automatically safe opioid threshold below which an ED prescription spares all patients from the hazard of risky or long-term use.” These findings are consistent with studies of opioid prescriptions in other settings and among other populations. A national study by Bao and colleagues last year found that the duration and dose of an initial opioid prescription were associated with high-risk subsequent use among privately insured and Medicare Advantage patients.
The good news is that fewer initial opioid prescriptions nationally are being written; one large study found a 54% decrease in the incidence of initial opioid prescriptions between July 2012 and December 2017. Although pain management remains important, providers are now looking to safer, non-opioid alternatives to do it.