Survey Results Reveal How Participants at Syringe Service Programs Decide on Treatment
Treatment choices were strongly shaped by convenience and the availability of health services.

In the U.S., as few as 1 in 8 individuals who inject drugs receives the necessary care to prevent or treat their substance use and related health conditions like wound infections, hepatitis C virus (HCV), or HIV. While syringe services programs (SSP) offer non-stigmatizing and low-barrier care, such as needle exchange, on-site HCV and HIV screening, wound care, and medication for opioid use disorder (OUD), there is limited understanding on how people who inject drugs (PWID) would like to receive those treatments.
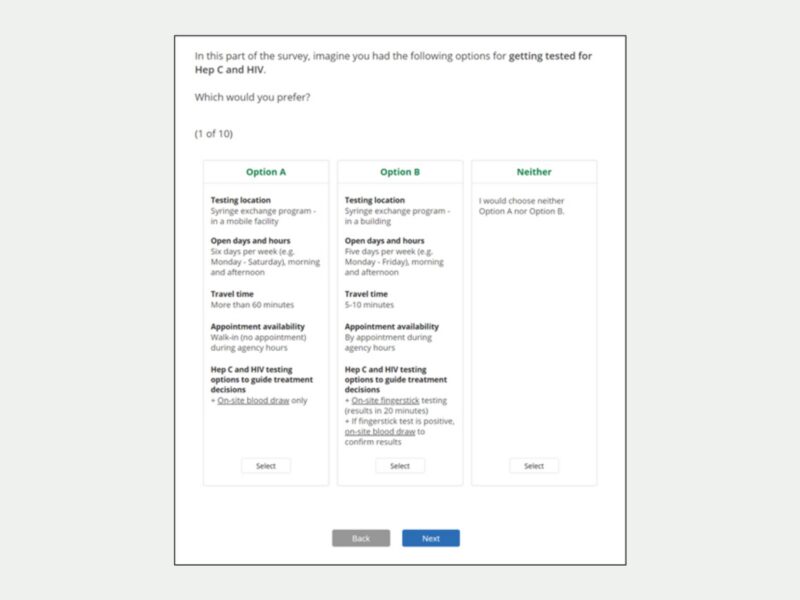
To improve healthcare engagement among PWID, lead author Rebecca Zimba and co-authors including CHERISH Director Bruce Schackman and CHERISH Research Affiliate Czarina Behrends conducted a discrete choice experiment (DCE) to understand SSP clients’ preferences for receiving care. Unlike the commonly used Likert scale, which asks respondents to rate how much they like or agree with an option, DCE is a survey design that asks participants to choose between alternative choices that simulate their decision making in the real world. DCE also has the advantage of measuring what preferences a respondent values and capturing how the strength of a preference influences their choices.

Czarina Behrends, PhD
Czarina Behrends, senior author, is an assistant professor in the Department of Population Health Sciences at Weill Cornell Medicine.
Between March 2023 to February 2024, a total of 546 participants were recruited from 14 SSP sites across 12 states to complete the survey. They were asked where and how they prefer to receive wound care, HIV/HCV screening, and buprenorphine treatment for OUD. The team used a latent class analysis to identify and select three groups that highlight distinct preference patterns for each health service.
Key Findings
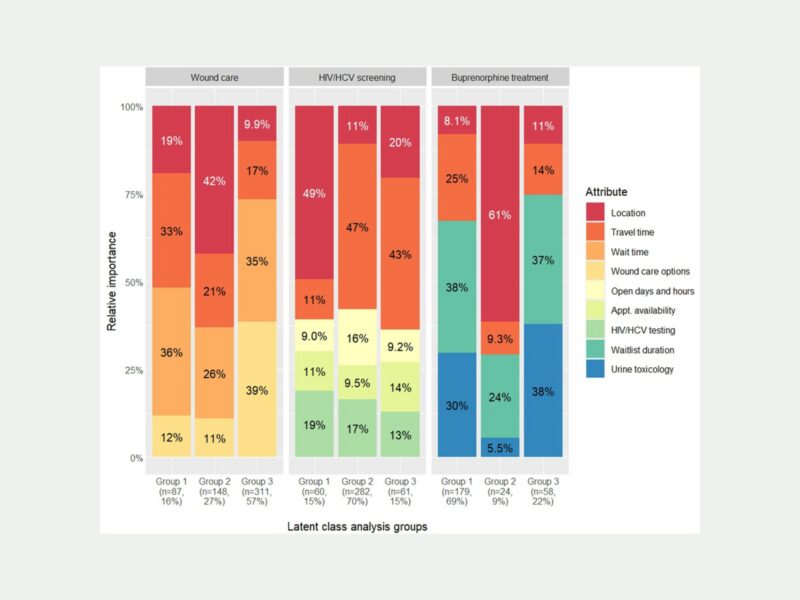
Across all three health services, the study captured strong preferences for ease of treatment access among most participants and a consistent preference for receiving treatment onsite at SSPs among a subset of participants.
- Across all services, participants valued shorter travel times, wait times, and waitlists. For each health service, more than one group showed preference for receiving on-site treatment at SSPs.
- Wound care groups differed by their strength of preferences for convenience (i.e., wait time, travel time), service location (i.e., SSP locations), and care comprehensiveness (i.e., first aid, oral antibiotic treatment, and wound lancing).
- All HCV/HIV screening groups preferred shorter travel time, and differed by strength of preferences for location (i.e., SSP locations), travel times, and testing options (i.e., on-site fingerstick testing with referral and on-site fingerstick testing with on-site blood draw).
- All buprenorphine groups preferred less punitive consequences for positive urine toxicology results (i.e., less frequent testing and having a treatment conversation if positive) and duration of the wait list (i.e., no wait list or <1 week waiting time), but differed by their preferences for locations.
Findings from the study illustrate that PWID have strong preferences for convenience and easy access to health services, and a subset of participants preferred receiving services in SSP settings. To guide the expansion or delivery of treatment for PWID, SSPs and traditional clinical settings may consider incorporating influential attributes into the services they provide, such as offering rapid on-site screening for HIV/HCV, allowing for walk-ins, reducing wait list times, expanding service locations, and implementing non-punitive and non-stigmatizing approaches. The authors also note that SSPs will need implementation and funding support to respond to these preferences by offering accessible medical services through telehealth, integrating on-site comprehensive health services, and delivering low-threshold buprenorphine treatment. Future research may examine how to optimally implement health services and deliver on the preferences identified by PWID in a variety of settings.
The study, “Syringe Services Participants’ Preferences for Wound Care, HIV/Hepatitis C Virus Screening, and Opioid Use Disorder Treatment: A Discrete Choice Experiment,” was published in Value in Health on November 19, 2025.