
Modeling infective endocarditis mortality associated with injection opioid use
Injection-related infective endocarditis (IE) is a serious and expensive medical complication among people who inject drugs (PWID). In some states, such as North Carolina there has been a 12-fold increase in injection-related IE between 2007 and 2017. Approximately 1.3% of people who inject drugs report IE within the past year, and between 0.5% and 11.8% report IE […]

Rapid versus Laboratory HIV and HCV testing for People Who Use Drugs
HIV outbreaks in Indiana, West Virginia, and Massachusetts have highlighted the need to rapidly identify and treat HIV infections among people who use drugs and their social networks in order to prevent disease transmission. Many state and local health departments have expanded their fourth generation laboratory-based HIV testing capacity that allows them to identify acute […]
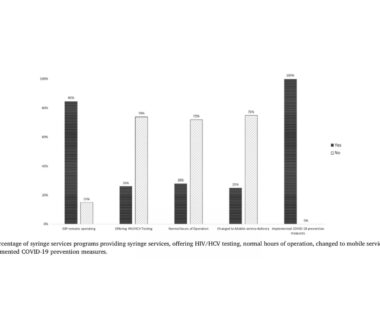
Effects of COVID-19 on Syringe Service Programs
They have increased prevalence of pre-existing co-morbidities that may increase their risk of a negative outcome following COVID-19 exposure, for example respiratory and cardiovascular diseases due to smoking cigarettes, marijuana, or other substances. Syringe service programs (SSPs) not only provide sterile injection equipment to PWUD, but also other health services such as HIV and hepatitis C […]

Patients Get More Opioids Than They Need After Knee Arthroscopy
In our new study in BMJ Open, we show that in 2015-2019 more than 70% of U.S. opioid-naive patients received an opioid prescription after knee arthroscopy. They received an average of 40 tablets, despite recent studies showing most patients end up taking less than 5 tablets. The take-home message? Despite recent attention to opioid stewardship, we find wide variation […]
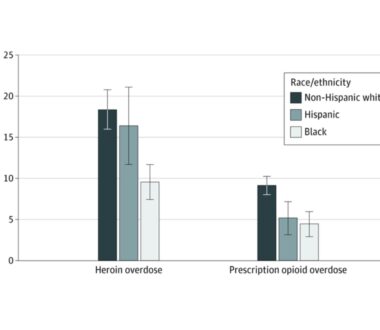
After Opioid Overdose Emergency, Few Patients Receive Timely Follow-up
An opioid overdose is significantly more than an isolated event. Patients who present to the emergency department (ED) with overdose have a 6 percent risk of dying in the following year. As with other high-risk acute conditions, we expect patients who survive overdose to receive evidence-based treatment after leaving the hospital. Whether the overdose was due to prescription […]

COVID-19 Can Change The Way We Respond To The Opioid Crisis – For The Better
The Coronavirus (COVID-19) pandemic has brought unprecedented challenges in healthcare delivery to people who use drugs. However, it may also have provided impetus to precipitate innovative changes in providing opioid overdose prevention, syringe services, and medication for opioid use disorder (MOUD) to this vulnerable population. In a new Viewpoint in Psychiatric Services, CHERISH Research Affiliate Yuhua Bao from […]

Simulation Modeling Presents Opportunities To Support The Public Health Response To The Opioid Crisis In North America
Although there are several evidence-based cost-effective interventions for people with opioid use disorder (OUD), they are underutilized. Questions remain regarding intervention selection, and cost of service delivery. Simulation modeling offers an opportunity to support decision making to address the syndemic of opioid overdose, HIV, and hepatitis C (HCV). In an article recently published in the International Journal […]
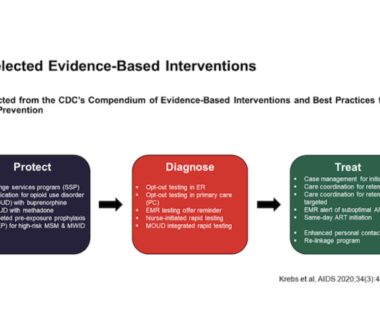
Optimizing HIV Prevention in Six US Cities: An Economic Model
In 2019, the United States launched the effort to End the HIV Epidemic by reducing new infections by 75% within 5 years and by 90% within 10 years. This national strategy comes with some new funding for the Centers of Disease Control and Prevention (CDC), the Health Resources and Services Administration (HRSA), and the Ryan White HIV/AIDS […]

Overdose and Re-hospitalization Rates Following Endocarditis Are Lower for Patients Receiving Medications for Opioid Use Disorder
The proportion of hospital admissions for endocarditis attributable to injection drug use increased from 7% in 2000 to 12% in 2013. Endocarditis is an infection in the lining of the heart chambers and valves that can be contracted through shared injection equipment. Rates of endocarditis are disproportionately affecting young people who inject drugs (PWID), which has […]

Will Eliminating Waiver Requirements Improve Access to Buprenorphine for Treating Opioid Use Disorder? Evidence From Increasing the Patient Treatment Cap
The Drug Addiction Treatment Act of 2000 (DATA 2000) permits qualified physicians to obtain a waiver to treat patients with opioid use disorder (OUD) with buprenorphine in office-based practices. In 2016, 47% of all US counties and 72% of rural counties lacked a buprenorphine waivered physician. That year, the Comprehensive Addiction and Recovery Act extended buprenorphine prescribing […]

Hospital Financial Incentives to Improve Care After Opioid Overdose
Early analysis of Pennsylvania’s program Two patients are treated for opioid overdose at two different hospitals, just a few miles apart. The first hospital provides life-saving treatment to reverse the overdose and watches the patient for an hour, discharging them when deemed “medically stable.” The second hospital also provides life-saving treatment but then offers counseling, […]

Methodology Consultation Success Story: Dr. Ashish Premkumar
The incidence of neonatal abstinence syndrome (NAS), also known as neonatal withdrawal syndrome, increased nationally from 3.4 per 1000 hospital births in 2009 to 5.8 in 2012. Recent estimates of NAS cost $1.5 billion dollars with the majority of the financial burden falling to state Medicaid programs. However, pregnancy offers a unique opportunity for women with […]
Engage with CHERISH
Submit a Consultation Request or Contact Us to learn more about how CHERISH can support your research or policy goals.